People with migraines experience many disruptions in their daily lives. Severe attacks can last for many hours or even days, causing you to miss important events or fall behind on work. You might also experience anxiety due to the uncertainty of the next attack.
Those with migraine might also have to manage multiple chronic conditions. Comorbidity occurs when you have more than one chronic disease simultaneously. You might have to balance migraine management with another condition, increasing the challenges of daily life.
Luckily, those with multiple comorbidities can find comprehensive treatment plans to help them manage their situations.
Understanding comorbidity
Comorbidity is the presence of two or more distinctive chronic medical conditions at one time. The two might interact with each other or remain separate — the multiple chronic conditions occur simultaneously but don’t necessarily cause the other.
Comorbidities exist for a variety of reasons, from genetic predisposition to general risk factors, and can involve your physical and mental health. For example, someone might have anxiety and then later develop arthritis. Arthritis would be known as comorbidity because they now have two chronic conditions at once.
Comorbidities can occur due to a variety of causes:
- Shared risk factors: Some diseases share risk factors, making you more likely to develop both at once. For instance, strokes and heart attacks both involve blood flow. Factors like high blood pressure, smoking and lack of physical exercise are risk factors for both strokes and heart attacks. If someone experiences multiple of these risk factors at once, they become more likely to experience a heart attack and a stroke.
- Shared causes: Comorbidities can have the same underlying causes. For instance, a person might have two autoimmune disorders, both of which target the immune system. Having one disease of a particular cause increases your risk of developing another.
- Direct causation: One chronic disease could directly cause another. For example, someone might develop depression as a result of another condition, like migraine.
Types of comorbidities
Comorbidities can impact many health areas. These are the types of comorbidities:
- Psychiatric: Psychiatric comorbidities largely involve your mental health. Some psychiatric comorbidity examples include depression, anxiety, post-traumatic stress disorder or panic disorder. These conditions can be present before another disease develops. Many people living with chronic diseases also struggle with their mental health. For example, one-third of individuals with lifelong conditions report symptoms of depression.
- Medical: Medical comorbidities affect the physical body. Examples include asthma, irritable bowel syndrome, sleep disorders, Chron’s disease and other pain conditions.
- Neurological: Neurological comorbidities impact your brain function. Examples include epilepsy, strokes, migraines, brain tumors and multiple sclerosis.
You might develop diseases of the same type or have diseases that fit multiple categories.
Comorbidity vs. complication
An important part of the comorbidity definition is its distinction from medical complications.
A complication is a side effect that occurs during a disease or after a treatment. For example, someone might encounter a complication during pregnancy that results in a miscarriage or stillbirth. In comparison, comorbidities are separate illnesses you can have in addition to the initial condition.
Get Drug-Free Migraine Relief With CEFALY
Shop Now
90-day money back guarantee
FDA-cleared
financing available
Comorbidities and migraine
Unfortunately, comorbidities are common for those with migraine. Experts have identified more than 75 conditions as confirmed comorbidities for migraine. Here are a few common examples:
- Anxiety: Anxiety is characterized by excessive fear and worry that disrupts your everyday life. Frequent symptoms include restlessness, impaired concentration, fatigue, hypervigilance or irritability. Anxiety disorders are up to five times more common for those with migraine than the general population. People with migraines might feel anxious about potential migraine attacks or when they encounter triggers.
- Back pain: Acute back pain is a common condition for many Americans, commonly in the lower back area. One study confirmed that those with migraine or chronic tension headaches were more than 1.5 times more likely to develop back pain. You might experience additional back pain during migraine attacks.
- Bipolar disorder: An example of a psychiatric comorbidity is bipolar disorder. This condition involves intense mood changes, from severe depression to euphoria. One study found that one-third of patients with bipolar disorder also had migraine attacks.
- Depression: Depression causes severe feelings of sadness that interfere with self-worth and daily motivation. Migraine and depression are commonly linked in patients. Migraine attacks cause intense pain and make many patients miss important life events and milestones, leading to feelings of frustration and hopelessness. Research reports that those with migraine are more than 2.5 times more likely to feel depressed.
- Epilepsy: Like migraine, epilepsy is a neurological condition. It’s characterized by regular seizures and has many genetic similarities to migraine development. Patients with migraine have an overall higher chance of developing epilepsy.
- Hypertension: Hypertension, or high blood pressure, is a common comorbidity for people with migraine.
- Insomnia: Insomnia is a sleep-based condition that impacts people’s ability to fall asleep or remain asleep throughout the night. One study found more than one-fourth of those with migraines also experience insomnia.

Treating migraine comorbidities
Finding the right treatment plan for migraine comorbidities is often a complicated process. Some medications might suit one condition but interfere with your migraine attacks, or migraine prescriptions might conflict with other conditions.
For example, triptans are common medications for migraine. They calm down overactive pain nerves in the brain, relieving pain during a migraine attack. However, triptans might conflict with other conditions, such as heart attacks. In cases like this, you’d have to develop an alternative treatment plan for migraine.
It’s beneficial to meet with a headache specialist or doctor to discuss a personalized comorbidity treatment plan. They can help you identify medications or other options that are safe for your comorbidities.
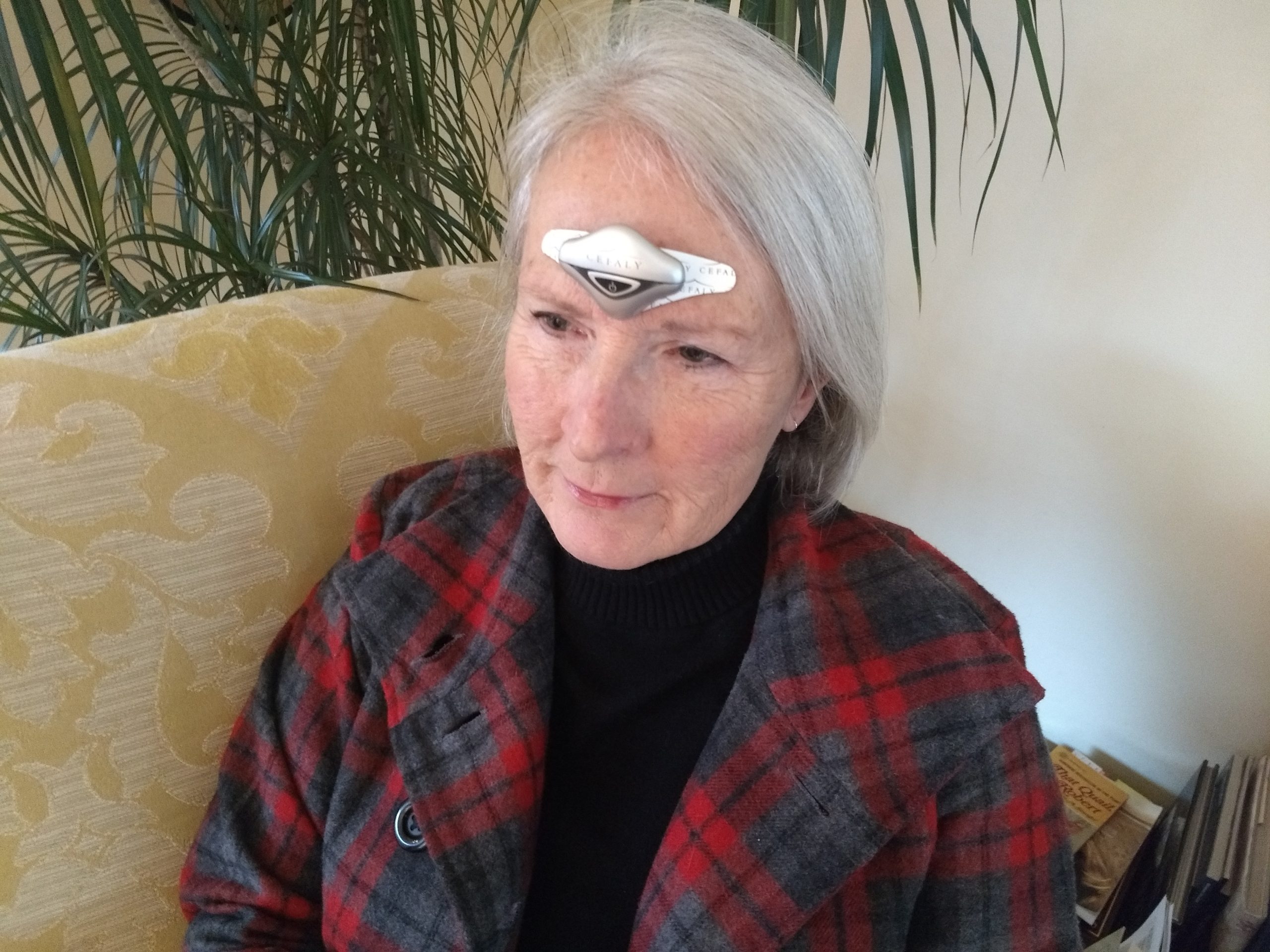
CEFALY is an alternative treatment device for migraine. This drug-free, clinically tested device can reduce migraine frequency and alleviate pain during attacks. It targets the trigeminal nerve, the primary pathway for pain during migraines. You can connect the device to the accompanying app, CeCe, to gain personalized insights into your attacks and symptoms.
CEFALY is an excellent option for comorbidity treatment because you can pair it with other condition medications.

Try CEFALY today
If you’re seeking migraine relief, choose CEFALY today. Our CEFALY Connected device uses external trigeminal nerve stimulation (eTNS) to desensitize your trigeminal nerve over time. You can wear CEFALY daily to lower attack frequency or put it on when an attack begins to reduce pain. The device can help you manage migraine comorbidities and reach a higher quality of life.
To get started with CEFALY, shop for our CEFALY Connected device today.