Managing migraine while receiving breast cancer treatment isn’t a simple process. To avoid drug interactions and harmful side effects, patients should work with their doctors on a tailored migraine treatment plan that includes more than medication. An effective migraine treatment plan will address triggers, lifestyle adjustments, and non-drug options for preventing and treating migraine, so you can feel better during your cancer treatment journey.
Breast cancer and migraine: What’s the connection?
Are people with migraine less likely to get breast cancer? Some studies have found this to be the case, although researchers aren’t clear on the reasons why. Migraine patients tend to use NSAIDs and avoid alcohol and smoking, and these habits can loser breast cancer risk. Hormones may also play a role, as migraine and breast cancer are both affected by estrogen.
Other studies have found an increased risk of breast cancer in migraine patients, while still other studies found no significant link at all.
Can breast cancer treatment cause migraine?
Yes. If you already have migraine, going through breast cancer treatment can make attacks more frequent or more severe. Even if you’ve never been diagnosed with migraine, you may start to experience symptoms once you start certain treatments.
- Hormonal therapy, which breast and prostate cancer patients may receive alongside chemotherapy, leads to hormonal fluctuations that can trigger headaches and migraine attacks.
- Some cancer medications may have migraine-inducing side effects or can aggravate migraine symptoms in patients who already suffer from them.
- Lifestyle factors such as poor sleep, dietary changes and less physical activity during treatment can contribute to migraine attacks.
- Stress and anxiety from a breast cancer diagnosis and treatment can also trigger migraine.
Get Drug-Free Migraine Relief With CEFALY
Shop Now
90-day money back guarantee
FDA-cleared
financing available
Migraine vs. other headaches caused by breast cancer treatment
An essential part of cancer treatment is managing side effects, which may include headaches. But how do you know if you have migraine?
Primary headaches, which include migraine, cluster headaches and tension headaches, don’t have an external cause. Secondary headaches are caused by medical conditions or medicine. To help your doctor diagnose your headache pain, make sure to mention:
- Location: Specify if the pain is in the forehead, temples, back of the neck or over the eyes.
- Quality: Describe how the headache feels, whether it’s pressure, a dull ache or a throbbing, stabbing or piercing pain.
- Severity: Is the headache mild, severe or incapacitating? Are you experiencing other symptoms?
The primary differences between a severe headache and a migraine attack are that a migraine typically includes other symptoms and is often debilitating. An attack may last for several hours or up to three days at a time. Symptoms like nausea, vomiting, or light and sound sensitivity can accompany a migraine attack. Patients may also develop warning signs of an impending migraine attack through aura. Visual auras can include fleeting bright lights or zigzag lines, while non-visual auras show up as tingling, numbness or abnormal fatigue.
A health care provider will analyze these patterns. They may order blood tests, a computed tomography (CT) scan or a magnetic resonance imaging (MRI) to rule out any additional health problems. Ask your health care team if headaches or migraine attacks are a common side effect of any prescription medications you’re taking as part of cancer treatment.
How to treat migraine headaches when you have cancer
Raising awareness among breast cancer patients about migraine triggers and symptoms can lead to early recognition and better management. Patients should keep a diary to identify potential external migraine triggers and what helps ease them. To see if there is a pattern, note the timing, frequency and duration alongside any triggers.

How to prevent migraine during cancer treatment
Avoid or limit exposure to triggers outside of your breast cancer treatment that contribute to migraines and headaches. One of the most powerful triggers is stress. To lessen the burden of emotional and physical stress during cancer treatment, try techniques like meditation and progressive muscle relaxation. Regular exercises like yoga, prioritizing self-care, getting social support or counseling sessions and breast cancer support groups can also help.
A few additional ways to prevent migraine headaches:
- Get enough sleep: A total of eight hours of sleep is crucial for cancer patients to support their treatment progress.
- Intentionally relax: A few times a day, stretch your neck, arms, legs and back to help your muscles relax.
- Eat regularly: Missing meals can lead to a headache. Avoid migraine-triggering foods, such as foods with tyramine (like aged cheeses) and foods made with nitrates (like lunch meats).
- Avoid caffeine: Additional caffeine can trigger headaches, so limiting intake or cutting out caffeine-containing soda, coffee or chocolate entirely is best.
- Drink enough water and electrolytes: Stay hydrated throughout the day, especially if the medication causes any nausea and vomiting.
- Medication adherence: Follow the treatments doctors prescribe and take medications consistently.
How to relieve migraine during cancer treatment
For cancer patients, experiencing debilitating headaches and migraines can add to an already demanding physical and emotional toll. It is vital to continue to practice self-care when headaches develop and to be proactive about pain management during an attack. Ask for help when pain levels rise. Loved ones can bring you your medication, assist you in moving to a darkened room for sensory relief, or provide physical and moral support. Other solutions to managing migraine headache:
- Cool compress: Use an ice pack or cool washcloth on the forehead, nape of the neck or temples to ease the pain. Some patients may use a cool compress on the forehead along with a warm compress on the neck or back of the head.
- Remove any stimuli: Lie in a quiet, dimly lit room and try to relax.
- See a physiotherapist: A physio can provide some helpful exercises or strategies to manage headaches and migraines in real time.
- Neuromodulation:
- Medication: Use prescription medication to treat symptoms.
- Hydrate: As with prevention, hydrating is vital to managing a headache or migraine attack.
- Ginger: Consume ginger by brewing it as a tea or drinking it as a concentrate supplement to help with pain and nausea.
- Doctor follow-up: Attend regular check-ups and discuss changes in symptoms, frequency or intensity of headaches and migraine attacks.
Relieve and prevent migraine without drugs: Try CEFALY
In the journey of managing cancer and its associated challenges, effective headache and migraine management becomes an essential aspect of comprehensive care. Migraine sufferers have a hypersensitive nervous system that overreacts to stimuli, leading to acute pain and neurological dysfunction. The trigeminal nerve, which branches throughout the head and face, is the primary conductor of migraine pain.
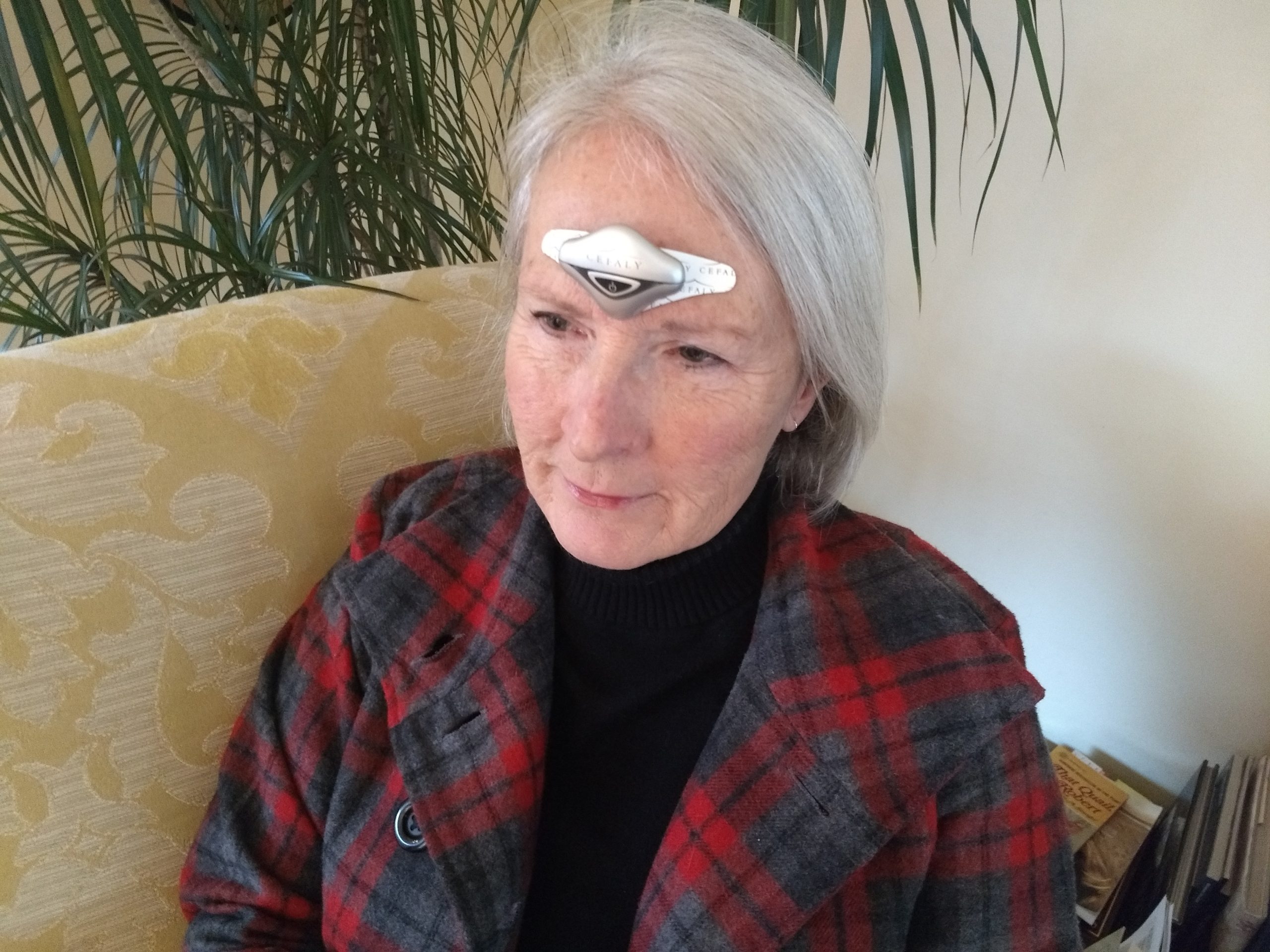
CEFALY uses gentle stimulation to desensitize this nerve. ACUTE treatment relieves migraine pain and other bothersome symptoms. Daily PREVENT treatments with CEFALY can reduce migraine frequency.
Learn How CEFALY Prevents & Relieves Migraine Pain
Discover the #1 FDA-cleared migraine treatment device
Try CEFALY risk-free for 90 days. Don’t love it? Just return the device for a refund.