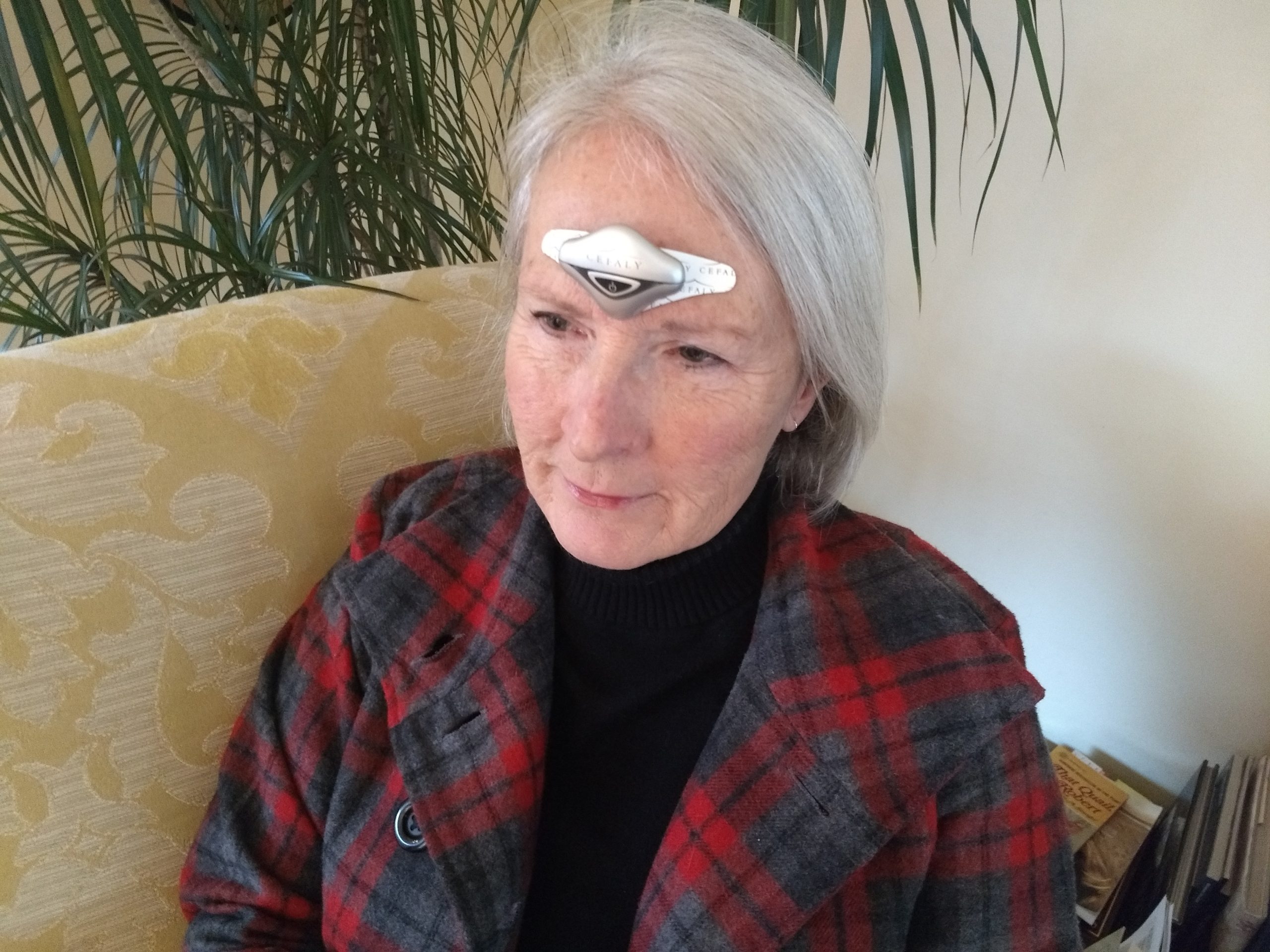
Finding out you’re pregnant can be one of life’s most joyful moments… but if you live with migraine, pregnancy brings so many new worries and questions. You wonder if your symptoms will get better or worse. You wonder how you can safely treat migraine in pregnancy without harming your unborn baby.
You’re not alone! Let’s look at some of the most common questions we hear about remedies and relief for migraine during pregnancy.
An important note: This blog is not medical advice. Always talk to your healthcare providers — both your OB/GYN and your neurologist or headache specialist — about any concerns or questions you have about treating migraine.
Does migraine get better during pregnancy?
This is the number-one question for most moms-to-be with migraine. The good news: almost half of women with migraine say their symptoms improve during the first trimester, and more than 80% of pregnant women with migraine experience fewer migraine attacks once they reach the second trimester. This may be due to rising estrogen levels.
(If you get menstrual migraine attacks, you’ve already experienced the effects of fluctuating hormone levels on migraine. Doctors believe that falling levels of estrogen before the menstrual period often cause migraine attacks in women.)
If your migraine frequency and severity get worse or stay the same during pregnancy, talk to your healthcare provider about ways to safely treat migraine.
Is migraine dangerous during pregnancy?
Even if you feel awful, migraine pain and other symptoms are not known to affect your unborn baby. However, some studies have shown that migraine is associated with a higher risk of pregnancy complications.
Researchers at Brigham and Women’s Hospital found that women with pre-pregnancy migraine were more likely to experience complications such as preterm delivery, gestational hypertension, and pre-eclampsia. “Our findings suggest that a history of migraine warrants consideration as an important risk factor for these complications and could be useful in flagging women who may benefit from enhanced monitoring during pregnancy,” said study author Alexandra Purdue-Smithe, associate epidemiologist at Brigham and Women’s Hospital and instructor in medicine at Harvard Medical School.
Get Drug-Free Migraine Relief With CEFALY
Shop Now
90-day money back guarantee
FDA-cleared
financing available
When should I contact a doctor about migraine headache symptoms during pregnancy?
Never hesitate to talk to your healthcare providers about any concerns you have during pregnancy, whether related to migraine or something else. It’s especially important to tell them about severe headache symptoms, which can be a warning sign of another serious condition.
Headache along with dizziness, blurred vision, or blind spots can be a sign that you have preeclampsia, a serious pregnancy complication. Some pregnant women with preeclampsia have symptoms similar to migraine—a throbbing headache with nausea and light or sound sensitivity. Call your doctor ASAP if you think you may have preeclampsia.
Other headache-related signs or symptoms that may indicate a serious pregnancy condition:
- Any new symptoms with your headache, such as changes in vision, aura, changes to speech or swallowing, weakness, numbness or tingling
- Any other change in your headache symptoms, frequency or severity
- An unusually severe or sudden onset headache (such as a “thunderclap” headache)
If you experience any of these symptoms, or if you’re having migraine symptoms for the first time during pregnancy, contact your healthcare provider right away.
Try CEFALY to Prevent & Relieve Migraine Pain
What are some safe ways to prevent migraine during pregnancy?
In general, doctors recommend using non-drug migraine prevention approaches when you’re pregnant. These healthy habits for migraine prevention can include:
- Avoiding triggers. If strong smells, bright lights, or certain foods often spark a migraine attack for you, do your best to steer clear.
- Eating balanced meals at regular times. It can be tough to do this if you’re feeling nauseous from pregnancy, but do your best to eat a variety of migraine-friendly foods.
- Drinking enough water — at least 64 ounces/2 liters of water each day
- Limiting caffeine. The general recommendation for pregnant women is to consume no more than 200 mg a day. Some women with migraine find that a small amount of caffeine is beneficial.
- Sticking to a sleep schedule. Going to bed and waking up at the same time each day is beneficial for migraine.
- Gentle physical activity, such as walking, swimming, or prenatal yoga
- Stress management techniques, such as meditation and relaxation
Practicing these migraine prevention techniques can raise your migraine trigger threshold: your default state of resilience. When your threshold is lower, you’re more sensitive to triggers and more likely to experience a migraine attack. Raise your threshold, and you can better withstand triggers.
Some pregnant women find that certain supplements can help with migraine prevention, such as magnesium and/or vitamin B12. Talk to your doctor before taking any supplements, even if they’re labeled “all-natural.”

What are some safe remedies for migraine during pregnancy?
The best place to start is with basic, drug-free migraine pregnancy relief techniques. Try using cold compresses and ice packs — not only on your head, but your neck as well. Rest in a dark, cool room. A small amount of caffeine may help.
If that’s not doing anything for your pain, get your healthcare provider to recommend pregnancy-safe migraine remedies. The American Academy of Family Physicians’ (AAFP) guidelines state that acetaminophen (Tylenol) and metoclopramide (an anti-nausea medication, branded as Reglan) are the only treatments for migraine that are considered safe in pregnancy.
What if your symptoms are more severe? “Although controversial, triptans can be considered for use in pregnant women with debilitating migraines when the potential benefits outweigh the risks,” the AAFP says. Some doctors may prescribe Fioricet, a combination of acetaminophen, butalbital, and caffeine.
Some migraine medications can be harmful when taken during pregnancy. For this reason, you should stop taking medication when you’re planning to become pregnant or when you find out that you’re pregnant.
Is CEFALY safe to use while pregnant?
CEFALY can be a safe and effective drug-free migraine treatment during pregnancy. Many women have used CEFALY for migraine relief during pregnancy with no known serious adverse effects. However, the safety and efficacy of CEFALY have not been evaluated in pregnant women. Ask your doctor before using CEFALY if you are pregnant or may become pregnant.
Curious about migraine treatment with CEFALY? Learn how it works. Then, try CEFALY risk-free with our 90-day guarantee!