Definitions of Migraine Terms
If you’ve recently been diagnosed with migraine, you may be overwhelmed by all the medical terminology. What’s MOH? What’s a silent migraine? What are all these medications people take?
We’ve put together a short and simple glossary to explain a few of the most common migraine terms you may read or hear.
Commonly Used Medical Migraine Terms & Definitions
Aura: Sensory disturbances that precede a migraine attack. The most common aura symptoms are visual — flashes of light, zigzag lines, bright spots or partial loss of vision. Aura may also include tingling sensations, numbness, limb weakness, or problems with speech and language.
Chronic migraine: Describes having a headache on 15 or more days per month, for more than months’ time, with at least eight of the headaches being migraines.
Episodic migraine: A type of migraine characterized by experiencing symptoms on fewer than 15 days each month.
Hemiplegic migraine: A type of migraine associated with weakness and/or loss of sensation on one side of the body.
Medication overuse headache (MOH): Painful, recurring headaches caused by the frequent use of pain medication. Migraine patients have a higher risk of developing MOH, which is also called rebound headache or medication adaptation headache.
Migraine: A neurological pain condition characterized by debilitating headaches as well as other symptoms, such as nausea, dizziness and sensitivity to light and sound.
Migraineur: A term for a person who has migraine. Many members of the migraine community prefer “person living with migraine.”
Neurologist: A doctor who specializes in disorders of the brain and nervous system, including migraine.
Ocular migraine: Migraine characterized by temporary loss of vision in one eye.
Pain management specialist: A doctor who specializes in treating all kinds of pain, including migraine pain.
Silent migraine: Migraine that does not cause headache pain but does include the other associated symptoms, such as aura, nausea, sensory changes, sensitivity to light and sound.
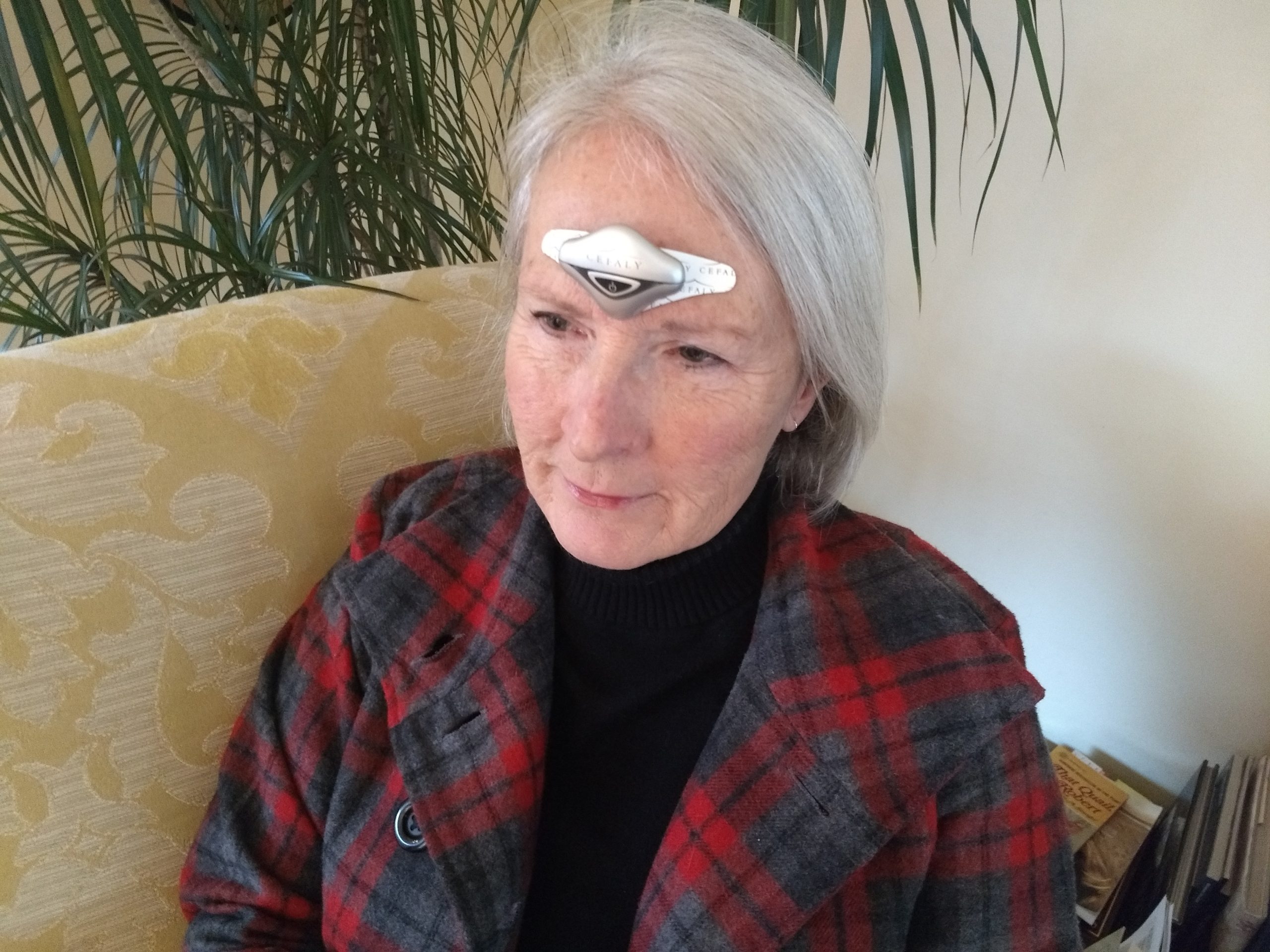
Trigeminal nerve: A large nerve in the head region which predominantly is responsible for sensation in the face and the sac that covers the brain. The trigeminal nerve has been shown in studies to be the primary site where migraines are activated and felt. CEFALY treats and prevents migraine headaches by targeting the trigeminal nerve.
Vestibular migraine: (additional names: migraine-associated vertigo; migraine-related vestibulopathy; migrainous vertigo) An episodic syndrome that may be associated with migraine, vestibular migraine is characterized by moderate to severe vertigo (dizziness), balance problems and/or motion sickness lasting between five minutes and 72 hours. Vestibular migraine can occur with or without the headache pain.
Stages of Migraine
Recent clinical research has identified headache pain as only one phase of a migraine. Scientists and clinicians have identified four phases of a migraine, each with its own characteristics.
Prodrome: (Also referred to as premonitory phase) The first phase of a migraine, which signals an oncoming attack and can last from hours to days. Prodrome symptoms may include constipation, diarrhea, irritability, fatigue, depression, food cravings and/or frequent yawning.
Aura: Sensory disturbances that occur for some, but not all persons experiencing migraine.
Pain phase: The throbbing, intense pain and other symptoms for which migraine is known.
Postdrome: The last phase of a migraine, which occurs after the pain has subsided and may last up to 48 hours. Postdrome symptoms may include fatigue, a continuing mild, dull headache, or (in some rare cases) euphoric feelings.
Treatments Used in Migraine
Anticonvulsants: Medications indicated and used to prevent or reduce symptoms of epilepsy. The medications topiramate (TPM) and valproic acid (VPA) have demonstrated positive treatment and are indicated for use for preventing migraine.
Antidepressants: Medications which are primarily used to treat symptoms of depression. Some research suggests two categories of antidepressants may help with migraine prevention and associated mood dysregulation symptoms. These antidepressants are the tricyclics and selective serotonin and norepinephrine reuptake Inhibitors (SNRIs). With both, 4-6 weeks are required before the effects of the medication are seen.
CGRP antagonists: A new type of preventive migraine medication that blocks reception of or binds to calcitonin gene-related peptide, a protein involved in the transmission of pain in the head.
Beta-blockers: A category of medication that is used to treat a variety of disorders. Originally, beta-blockers were used to treat some heart disease and high blood pressure, but they have also been shown to be effective in treating other disorders such as migraine. These medications target your heart and blood vessels to help prevent the onset of migraine. The current theory of how these medications work with migraine is that they reduce the dilation associated with a migraine attack. Examples of beta-blockers are atenolol, metoprolol, propranolol, nadolol and timolol. Be sure to inform your healthcare provider if you have asthma, Raynaud’s syndrome or COPD before taking a beta-blocker.
OnabotulinumtoxinA: A toxin produced by Clostridium botulinum, onabotulinum A is used therapeutically as an injectable, preventive treatment for chronic migraine headaches. Originally introduced as a cosmetic treatment to reduce wrinkles, onabotulinum A is thought to work in migraine by blocking the nerve signals that cause blood vessel dilation.
Calcium channel blockers: Another medication used in cardiovascular treatment, calcium channel blockers reduce blood vessel constriction and are used by some physicians when other preventive migraine medications have not worked. The two most used are flunarizine and verapamil.
Ergotamine: (also dihydroergotamine or the “ergots”) Ergots were the cornerstone of acute migraine treatment before the introduction of triptans. Ergotamines work by constricting blood vessels around the brain.
NSAIDs: Nonsteroidal anti-inflammatory drugs that can help to reduce migraine pain. Common over-the-counter NSAIDs include ibuprofen (e.g. Advil) and naproxen (e.g. Aleve).
eTNS: External trigeminal nerve stimulation, a non-invasive method of neuromodulation. The CEFALY device uses eTNS to send tinyimpulses through an electrode positioned on the forehead to modify pain transmission and processing in the trigeminal nerve.
Occipital nerve block: A procedure where your healthcare providers injects a combination of a local anesthetic and anti-inflammatory drug at the base of the skull, resulting in temporary pain relief. While pain relief onset occurs in a matter of minutes, nerve blocks typically wear off in one to two weeks but can also last for months in a few patients.
Triptans: The first-line therapy prescribed by healthcare providers for acute migraine treatment outside of an urgent setting. Triptans are highly specific for stimulating a subtype of receptor for serotonin. These specific serotonin sites are primarily located in the vessels around the brain, and so triptans are thought to reduce inflammation and constrict these vessels, alleviating migraine pain.
Any terms you’d like to learn more about? Email us here and ask!
Get Drug-Free Migraine Relief With CEFALY
Shop Now 


90-day money back guarantee

FDA-cleared

financing available
Get Drug-Free Migraine Relief With CEFALY
Shop Now
90-day money back guarantee
FDA-cleared
financing available
Migraine 102: More Migraine Terms You Should Know
After you’re diagnosed with migraine, you’ll discover that the world of migraine treatment options is vast and sometimes confusing. Migraine communities offer spirited discussions and warm support, but newcomers might wonder: What does HYH stand for? And why is everyone talking about pies and toolboxes?
We wrote this follow-up to our Migraine 101 Glossary to explain some migraine terms you may encounter.
14 More Migraine Terms to Know
Abortive Medication: This type of medication is taken at the very first sign of an attack, with the goal of stopping migraine symptoms from developing.
CoQ10: Often abbreviated as CoQ or CoQ10, coenzyme Q10 is an antioxidant produced naturally by the body. Some people find that taking CoQ10 as a supplement can help reduce migraine frequency.
Green Light Therapy: Some new research has shown that exposure to green light, at a specific frequency and intensity, may help reduce headache days and pain intensity.[i]
HYH: This is one of the migraine terms you’ll see all the time in migraine community posts — so what does HYH mean? It’s an abbreviation for the “Heal Your Headache” migraine prevention diet, first developed by Dr. David Buchholz, MD. This diet seeks to eliminate migraine-triggering foods and additives, including (but not limited to) chocolate, nuts, citrus fruits, processed meats and fresh-baked breads.
Integrative Approach: An integrative approach to migraine treatment takes a holistic view that includes mind, body, spirit and community. “Integrative medicine neither rejects conventional medicine nor accepts alternative therapies uncritically,” explains the Andrew Weil Center for Integrative Medicine at the University of Arizona.
Keto: This refers to the ketogenic diet, a high-fat, minimal-carb diet that has been shown to relieve migraine attack frequency in some people. Learn more about keto for migraine.
Magnesium: Magnesium is a naturally occurring mineral that plays a crucial role in more than 300 enzyme systems in the body. According to the National Institutes of Health, “several small studies found that magnesium supplements can modestly reduce the frequency of migraines.” [ii] Many people with migraine find that taking a magnesium supplement helps, although it can also cause stomach upset.
Migraine Toolbox/Toolkit: A migraine toolkit is a collection of items that can help relieve pain and make you feel better during an attack. Your toolkit might include sunglasses, water, ice packs, migraine medication and your CEFALY DUAL. Read more: What’s In a Migraine Toolkit?
Preventive Medication: This category includes any medications taken to reduce attack frequency and severity.
Rescue Medication: Rescue drugs are taken if abortive medication fails to stop a migraine attack. Rescue meds can’t make an attack end sooner, but they are intended to relieve pain, nausea and vomiting.
SEEDS: This mnemonic stands for five lifestyle modifications that can help migraine: sleep, exercise, eat, diary, and stress.
Spoon Theory: Christine Miserandino invented “spoon theory” as a way to show a friend what it’s like living with lupus. She placed 12 spoons in her friend’s hands, representing the energy and ability she had on an average day. She explained that everything she did took away a spoon; that her life was spent calculating the cost of every action.[iii] This story resonated so strongly that many people living with chronic illness, including migraine, have adopted Spoon Theory and call themselves Spoonies.
Treatment Pie: A concept developed by Migraine Strong, the treatment pie represents the nine facets of an effective migraine treatment program. “When applied together, they have a greater chance of reducing the frequency and severity of migraine attacks than any one slice alone,” the site explains.[iv] The nine slices are: Medications, Hydration, Meditation, Therapy, Sleep, Diet, Movement, Supplements and Miscellaneous.
Trigger: A migraine trigger is anything that sparks an attack. Triggers are highly individualized, but commonly include stress, weather, alcohol, certain foods, strong fragrances, bright lights and hormone changes.